Exercise stress test (exercise ECG): protocols, evaluation & termination
Exercise stress test (exercise ECG) protocols & equipment: cycle ergometer (bicycle) vs. treadmill
The choice of exercise equipment and protocol depends mainly on local traditions. The treadmill and cycle ergometer (bicycle) are the most frequently used test methods. Cycle ergometer is preferred in Europe, while treadmill testing is predominant in the United States. Treadmill and cycle ergometer both have their advantages and disadvantages, which will be discussed below. The basic principles of exercise test protocols will also be discussed in this article.
Metabolic equivalent (MET): measuring oxygen consumption
Estimation of oxygen consumption is central to the assessment of exercise capacity. Metabolic equivalents (METs) can be used to estimate the energy cost of physical activity. One metabolic equivalent (1 MET) is defined as the amount of oxygen consumed while sitting at rest and is equal to 3.5 ml O2 per kg weight × min. Metabolic equivalents are used because the concept offers an easy way of expressing the energy cost of any exercise. The energy cost is expressed as multiples of the resting metabolic rate. For example, 5 METs imply that the energy cost of activity is equal to five times the energy consumption at rest (sitting). METs may be used to describe the functional capacity during exercise stress testing. Results of treadmill tests are typically described in METs, whereas energy expenditure during bicycle ergometry is typically expressed in kilopond meters per minute. Note that kilopond meters per minute can be converted to Watts (1 kilopond meter per minute = 0.1634 Watts).
Protocols for clinical exercise testing generally include an initial warm-up period (at a low workload), followed by a successive (graded) increase in workload. The increase in workload occurs with predefined time intervals. A recovery period, during which the patient is still carefully observed, follows after the exercise effort is terminated.
Reliability as a function of workload
In order for the exercise test to be reliable, the patient must perform maximally, without risking serious complications. The instructor may facilitate this by supporting and motivating the patient during the entire procedure. If the achieved workload is not sufficient, the reliability and thus usefulness of the test will be inadequate. The whole purpose of the exercise ECG is to provoke physiological reactions that are not noticeable at rest. Hence, the examination may only be considered conclusive if the achieved workload is sufficient to provoke symptoms/signs that are not noticeable during rest. As a rule of thumb, the patient must achieve 85% of the (age-adjusted) expected maximum heart rate, which can be estimated using the following formula:
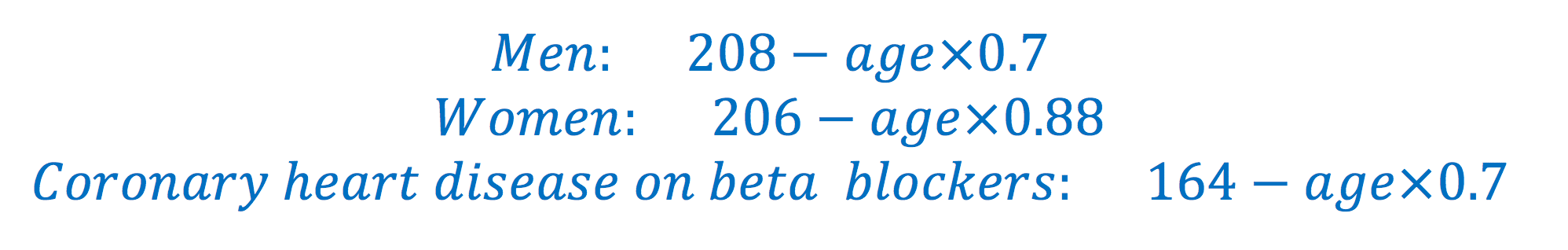
Accordingly, a 65-year-old male is estimated to have a maximum heart rate of 208-65×0.7, which equals approximately 163 beats per minute; and 85% of 163 is roughly 140. That male should therefore achieve a heart rate of 140 beats per minute for the exercise test to be reliable.
It should be noted that 85% is an arbitrary number and the exercise test must never be terminated once the patient has reached 85% of the expected maximum heart rate. The reasons for this follows:
- There is substantial individual variation in maximum heart rate. The standard deviation for maximum heart rate is around 10 beats per minute, which means that if the expected maximum heart rate is 160 min according to the equations above, it may actually be anywhere between 140 and 180 beats per minute.
- Patients with significant heart disease (known or unknown) may not achieve the expected maximum heart rate and it may be hazardous to push them towards it.
It is therefore recommended that the 85% cut-off be used only as a guiding principle rather than an absolute rule.
Evaluation of the exercise stress test: Parameters to assess
Evaluation of the exercise stress test is based on several parameters which must be assessed continuously during the procedure. These parameters are listed in the table below and discussed in detail in subsequent chapters.
| PARAMETER | COMMENT |
| General appearance | The presence of chest discomfort (pain) must be assessed repeatedly during the test. The severity of chest pain is graded from 0 (no pain) to 10 (maximal pain). |
| Chest discomfort (pain) | Maximal workload achieved and duration of the test |
| Dyspnoea/dyspnea and exercise effort | Leg fatigue is graded from 0 (none) to 10 (maximal. |
| Leg fatigue | Leg fatigue graded from 0 (none) to 10 (maximal. |
| Maximal workload acheived and duration of the test | Workload is expressed in METs, Watts, kpm, depending on protocol and test method. |
| Heart rate | Maximal heart rate is noted during the entire procedure (including the recovery period). Heart rate acceleration is also noted. |
| EKG/ECG reaction | Systolic blood pressure is measured every other minute. It is also measured at the termination of exercise and then every other minute during the recovery period. Automatic blood pressure monitor should not be used; measurements should be manual. |
| Blood pressure reaction | Systolic blood pressure is measured every other minute. It is also measured at the termination of exercise and then every other minute during the recovery period. An automatic blood pressure monitor should not be used; measurements should be manual. |
| Cause of termination | If the exercise test is terminated prematurely, the cause must be noted. |
Evaluation of ECG / EKG reaction
A 12-lead ECG is recorded at rest before the exercise test begins. That initial ECG is used as a baseline ECG and all subsequent ECGs (recorded during exercise) will be compared to it. In order to reduce artifacts from muscles and movements the ECG machine presents a signal-averaged ECG, which means that several consecutive ECG curves (waveforms) are averaged, which yields a clearer ECG curve. These signal-averaged ECG curves are continuously updated so that the clinician can monitor ECG changes in real-time. Note that the ECG machines detect ventricular extrasystoles (premature ventricular beats) and exclude them from the signal-averaged ECG. A separate rhythm strip is always available so that the clinician can monitor the frequency of ventricular extrasystoles.
ECG changes and their implications will be discussed in detail in subsequent articles.
The recovery period after termination of exercise
The recovery period starts immediately once the patient stops cycling/running. The patient is placed in the supine position which increases the venous return to the heart. The increased venous return will subsequently increase cardiac preload (a greater blood volume is returned to the left ventricle). Increased preload causes increased workload on the myocardium of the left ventricle and that may provoke myocardial ischemia due to increased oxygen consumption in the myocardium. Some patients only display ischemic ECG changes during the recovery period. Note that ECG recording continues during the entire recovery period, which is usually 6 to 8 minutes. The exercise test is terminated once all parameters (listed above) have returned to baseline values.
Termination of exercise
The exercise test is terminated when (1) symptoms are limiting the patient from continuing; (2) when formal termination criteria are fulfilled (defined below) or (3) when the test is completed.
Termination criteria
A plethora of studies conducted in the past few decades show that exercise stress testing is a safe procedure. The risk of complications is low, despite the fact that many participants have significant heart disease, including ischemic heart disease. However, one must always conduct tests with caution and terminate the test if the risk of complications is elevated. Hence, there are absolute and relative criteria for terminating a stress test.
Absolute termination criteria
The exercise test should be terminated in each of the following scenarios:
- ≥10 mmHg drop in systolic blood pressure in the presence of other signs suggestive of myocardial ischemia.
- Systolic blood pressure >280 mmHg. This limit is lower if the patient has an increased risk of bleeding (e.g. patients on anticoagulants).
- Pronounced angina pectoris (grade 5 or higher according to the visual analogous scale).
- Dizziness, pre-syncope, or more severe neurological signs.
- Cyanosis, paleness.
- Patient’s desire to terminate.
- Technical problems make ECG recording or blood pressure recording unreliable.
- Ventricular tachycardia (VT) with duration >30 seconds.
- Supraventricular tachyarrhythmia (tachycardia) with negative hemodynamic effects.
- ST segment elevation 1 mm or higher in leads without (pre-existing) significant Q-waves.
- ST segment depression >2 mm in two or more contiguous leads.
Relative termination criteria
In each of the scenarios listed below, one should consider terminating the test:
- ≥10 mmHg drop in systolic blood pressure (without other signs of myocardial ischemia).
- >115 mmHg diastolic blood pressure.
- Marked change in the electrical axis (ECG).
- AV (atrioventricular) block II, AV block III.
- Multifocal premature ventricular beats (extrasystoles).
- Frequent coupled premature ventricular beats.
- Bradyarrhythmia (bradycardia).
- Exhaustion.
- Leg cramp

