Premature ventricular contractions (premature ventricular complex, premature ventricular beats)
Premature ventricular contractions (premature ventricular complex, premature ventricular beats): ECG and clinical implications
Premature ventricular complexes are also referred to as premature ventricular beats, premature ventricular contractions or just ventricular beats/contractions/complexes. These terms will be used interchangeably in this discussion.
A premature ventricular complex is recognized on the ECG as an abnormal and wide QRS complex occurring earlier than expected in the cardiac cycle. It is caused by an impulse discharged from an ectopic focus which may be located anywhere in the ventricles. The ectopic impulse depolarizes the ventricles; because the impulse is discharged in the ventricles it will spread partly or entirely outside of the conduction system and thus produce a wide QRS complex (QRS duration ≥0.12 s). Refer to Figure 1 for an example.
The premature ventricular impulse replaces a sinus beat and induces a delay to the next sinus beat (the RR interval is increased after a premature ventricular complex). This yields more time to fill the ventricles with blood (increased ventricular filling). The person with premature beats might perceive this as palpitations, because of the stronger ventricular contractions caused by the increased filling.
Ventricular premature complexes are not preceded by P-waves because the ectopic impulse originates in the ventricles and does not influence the atria (with exceptions discussed below).
Although premature ventricular contractions are mostly harmless, they may trigger sustained ventricular tachyarrhythmias. This will also be discussed later.
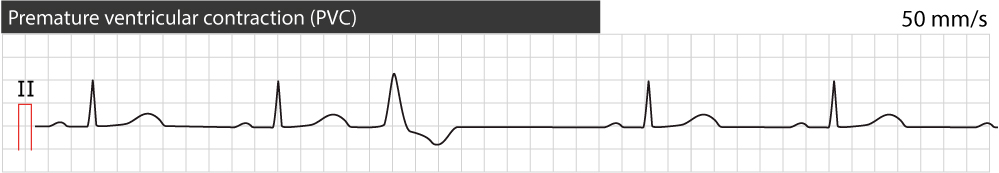
The impulse discharged from an ectopic focus in the ventricles will spread abnormally (because the impulse did not enter the ventricles through the bundle of His). Abnormal depolarization will consequently lead to abnormal repolarization. This explains the secondary ST-T changes seen on premature ventricular complexes; the ST-T vector will be directed oppositely to the QRS vector. As seen in Figure 1 the premature ventricular complex displays a positive QRS complex followed by a negative ST-T segment. Thus, the ST-T segment is directed oppositely to the QRS (this is called discordant ST-T segment).
Ventricular premature contractions and the complete compensatory pause
A premature ventricular contraction is followed by a complete compensatory pause which means that the next sinus beat will occur on schedule. The interval between the sinus beats occurring before and after the premature beat will be two sinus cycles (2 RR intervals). This is explained by the fact that the premature ventricular impulse does not discharge and reset the sinoatrial node, which will therefore continue on schedule. Refer to Figure 2.
Classification of premature ventricular contractions
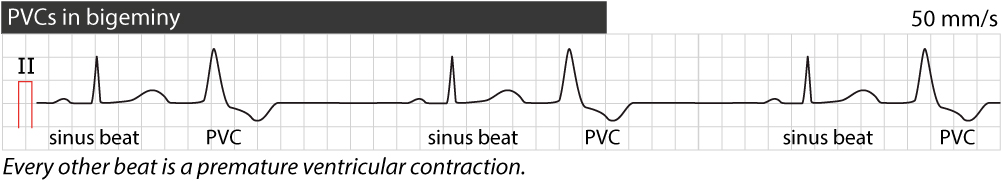
When every other beat on the ECG is a premature ventricular complex (PVC), the rhythm is referred to as PVC in bigeminy (Figure 3). If every third beat is a PVC, it is referred to as PVC in trigeminy. Similarly, there can be quadrigeminy and so on.
Two consecutive premature ventricular contractions are referred to as a pair or couplet. If 3 to 30 premature ventricular contractions occur consecutively, it is referred to as non-sustained ventricular tachycardia (if the rate is >100 beats/min) or ventricular rhythm (if the rate is <100 beats/min). If more than 30 consecutive beats are premature ventricular contractions it is referred to as sustained ventricular tachycardia if the rate is >100 beats/min.
Premature ventricular complexes discharged by the same ectopic focus will typically have similar morphology (appearance) and constant timing. Such premature ventricular complexes are referred to as monomorphic (or unifocal). This is exemplified in Figure 3.
Polymorphic premature ventricular complexes display constant timing but varying morphology. These beats typically originate in the same ectopic focus but the spread of the impulse (from that ectopic focus) varies from one beat to another (Figure 4).
Multifocal premature ventricular complexes have varying morphology and varying timing. These beats are discharged by several ectopic foci in the ventricles (Figure 5).

It is also possible to determine where the ectopic focus is located by assessing the morphology of the premature beat in lead V1. If the morphology in lead V1 is similar to a right bundle branch block (i.e predominantly positive), the ectopic focus is located in the left ventricles. If the morphology in lead V1 is similar to a left bundle branch block (i.e predominantly negative), the ectopic focus is located in the right ventricles.
Fusion beats
If a normal atrial impulse is conducted to the ventricles approximately simultaneously as a premature ventricular impulse is discharged, the ventricles might be depolarized by both these impulses. This typically occurs if the premature ventricular impulse is discharged late, around the time of the normal sinus impulse. The morphology resulting QRS complex will resemble a combination (a fusion) of the normal beat and the PVC. Refer to Figure 6.
Exceptions from complete compensatory pause
Although the complete compensatory pause is very typical of the premature ventricular complex (PVC), there are instances where it does not occur.
- Interpolated PVC: If a PVC occurs early after a normal beat, the atrioventricular conduction system might have repolarized by the time the next sinus impulse is discharged (this impulse is usually not conducted to the ventricles due to refractoriness in the atrioventricular conduction system), whereby the atrial impulse will reach the ventricles and depolarize them. This is called an interpolated PVC and it appears on the ECG as a PVC occurring between two sinus beats and there are no beats replaced and no pause.
- Retrograde atrial activation: Occasionally the ventricular impulse may be conducted backwards through the bundle of His into the atria and depolarize both the atria and the sinoatrial node. This resets the clock of the sinoatrial node. The next sinus beat will occur one sinus cycle after resetting the sinoatrial node. The pause will be less than compensatory and the retrograde P-wave is often visible on the ST-T-segment.
- Ventricular echo: This is a rare phenomenon in which the impulse from the PVC is conducted through the atrioventricular node and there it circulates back to the ventricles which are activated again. This yields a couplet with less than compensatory pause.
Clinical relevance of premature ventricular contractions
Premature ventricular contractions are common among both healthy individuals and there is robust evidence that do not affect long-term cardiovascular prognosis among those individuals. Premature ventricular complexes are even more common among individuals with heart disease. Premature ventricular complexes can be debilitating, even for healthy individuals.
Healthy persons
Almost 30% of all healthy individuals display premature ventricular contractions during exercise stress testing. Male sex, stress, nervousness, tobacco, coffee, hypokalemia, infection, alcohol, sleep deprivation and certain drugs are associated with increased occurrence of premature ventricular beats. Moreover, the frequency of premature beats increases with age.
Healthy individuals might display premature ventricular complexes on ECG during screening. It may be symptomatic or asymptomatic. Palpitations and the feeling that the heart “skips a beat” are common symptoms. Chest or throat discomfort is less common.
A few premature ventricular contractions daily in otherwise healthy individuals are considered benign and do not affect cardiovascular prognosis. However, if ventricular premature beats make up a significant proportion of all heartbeats during the day, the situation is more problematic. If >15% of all beats are premature ventricular beats there is a risk of PVC-induced cardiomyopathy and left ventricular dysfunction. In such cases it is wise to refer to patient for invasive examination; it is often possible to eliminate the ectopic focus (foci) using ablation therapy. This can also reverse established cardiomyopathy.
Persons with heart disease
Premature ventricular beats are common among those with heart disease. The frequency of premature beats is increased in a wide range of conditions, such as ischemic (coronary) heart disease. These individuals are generally more affected by premature beats, as they already have compromised cardiac function. Because premature ventricular beats have ineffective ventricular contraction, it can reduce cardiac output and thus cause deterioration of ischemic heart disease and heart failure.
R-on-T phenomenon
R-on-T phenomenon has been discussed here.
Treatment of premature ventricular contractions
Underlying heart disease must be ruled out among persons without previously known heart disease. The procedure must be individualized and guided by ECG, anamnesis and findings from physical examination. Rather few otherwise healthy individuals necessitate treatment. Among those with heart disease, the proclivity to treat should be higher. Before treatment is instigated, it is important to analyze potassium and magnesium levels because hypokalemia and hypomagnesemia may cause PVCs and these causes are reversible.
Treatment is instigated if (1) symptoms are significant, (2) of PVCs make up a significant portion of all beats during the day (examined with Holter-ECG), or (3) if the PVCs have a negative hemodynamic effect. The first choice of drug is beta-blockers (bisoprolol 5–10 mg once daily or sustained-release metoprolol 50–100 mg once daily). However, beta-blockers are often insufficient and symptoms may persist. Class I antiarrhythmic drugs can be tried, as can amiodarone. One should have invasive treatment with ablation in mind.

