Tamponade and cardiac arrest
Cardiac arrest associated with tamponade has an exceptionally poor prognosis. In the vast majority of these cases, the tamponade develops acutely or subacutely. It is uncommon for chronic pericardial effusions to cause sudden cardiac arrest since these cases tend to be recognized and managed before circulatory collapse occurs. The leading causes of cardiac tamponade culminating in cardiac arrest include:
- Aortic dissection: The proximal 4-5 cm of the aortic root is covered within the pericardium. Consequently, a proximal dissection can result in hemorrhage within the pericardium.
- Ventricular rupture: A transmural infarction can cause a rupture in the left ventricular free wall.
- Mediastinal trauma: Penetrating injuries to the mediastinum can cause tamponade.
- Post-operative Complications: Post-surgical complications following thoracic procedures can cause tamponade.
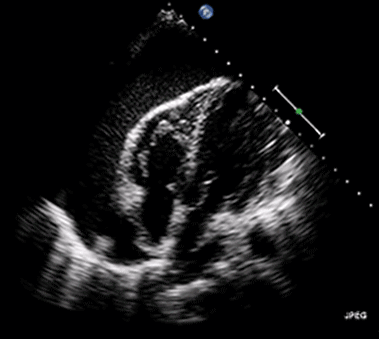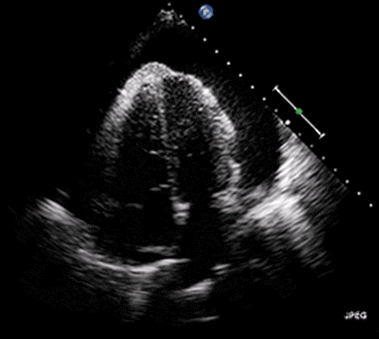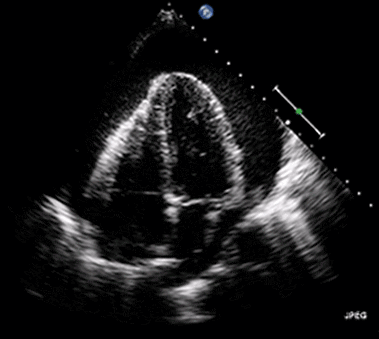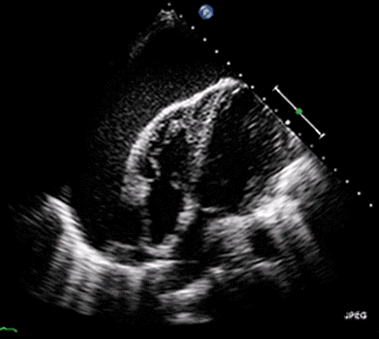
Rapid diagnosis of cardiac tamponade is possible via bedside echocardiography. This reveals pericardial fluid, suggesting hemorrhage in the context of cardiac arrest cases. Highly echogenic fluid indicates that the blood has coagulated, making it very challenging to drain using pericardiocentesis.
In cases of cardiac tamponade, conventional chest compressions are ineffective. This is explained by the elevated intrapericardial pressure due to the tamponade. The increased pressure causes compression of the atria and the ventricles (particularly the former). Even small pressure elevations on the right side can compromise venous return to the right ventricle. Therefore, in the presence of a tamponade, chest compressions have limited efficacy. Furthermore, administering large tidal volumes might inadvertently elevate intrathoracic pressures, additionally compromising venous return. Draining the pericardium, therefore, takes precedence over compressions.
For traumatic tamponades, thoracotomy remains the primary therapeutic intervention. Ideally, it should be performed within 15 minutes of the onset of collapse.
Pericardiocentesis, performed using a large needle introduced either via the subxiphoid or apical window, is generally considered less effective than thoracotomy. This is because it does not ensure complete drainage of the pericardium, and needles or catheters are at risk of bending or damage during chest compressions.
References
DeBehnke DJ, Hilander SJ, Doubles DW, Wickman LL, Swart GL. The hemodynamic and arterial blood gas response to asphyxiation: a canine model of pulseless electrical activity. Resuscitation 1995; 30:16975.
Safar P, Paradise NA, Weil MH. Asphyxial cardiac arrest. In: Paradis NA, Halperin HR, Kern KB, Wenzel V, Chamberlain DA, editors. Cardiac arrest—the science and practice of resuscitation medicine.
Kitamura T, Kiyohara K, Sakai T, et al. Epidemiology and outcome of adult out-of-hospital cardiac arrest of non-cardiac origin in Osaka: a population-based study. BMJ Open 2014; 4:E006462.
Deasy C, Bray J, Smith K, et al. Hanging-Associated out-of-hospital cardiac arrests in Melbourne, Australia. Emerg Med 2013; 30:3842.
Luna GK, Pavlin EG, Kirkman T, Copass MK, Rice CL. Hemodynamic effects of external cardiac massage in trauma shock. J Trauma 1989; 29:1430-3 .
Jeffcoach DR, Gallegos JJ, Jesty SA, et al. Use of CPR in hemorrhagic shock, a dog model. J Trauma Acute Care Surg 2016; 81:27-33 .
Watts S, Smith JE, Gwyther R, Kirkman E. Closed chest compressions reduce survival in an animal model of haemorrhageinduced traumatic cardiac arrest. Resuscitation 2019; 140:37-42.
Endo A, Kojima M, Hong ZJ, Otomo Y, Coimbra R. Open-chest versus closed-chest cardiopulmonary resuscitation in trauma patients with signs of life upon hospital arrival: a retrospective multicenter study. Crit Care 2020; 24:541.
Ebo DG, Clarke RC, Mertes PM, et al. Molecular mechanisms and pathophysiology of perioperative hypersensitivity and anaphylaxis: a narrative review. Br J Anaesth 2019; 123:e3849.
Wallmuller C, Meron G, Kurkciyan I, et al. Causes of in-hospital cardiac arrest and influence on outcome. Resuscitation 2012; 83:120611.
Wang CH, Huang CH, Chang WT, et al. The effects of calcium and sodium bicarbonate on severe hyperkalaemia during cardiopulmonary resuscitation: a retrospective cohort study of adult in-hospital cardiac arrest. Resuscitation 2016; 98:10511.
Saarinen S, Nurmi J, Toivio T, et al. Does appropriate treatment of the primary underlying cause of PEA during resuscitation improve patients’ survival? Resuscitation 2012; 83:81922.
Mroczek T, Gladki M, Skalski J. Successful resuscitation from accidental hypothermia of 11.8 degrees C: where is the lower bound for human beings? Eur J Cardiothorac Surg 2020; 58:10912.
Stephen CR, Dent SJ, Hall KD, Smith W.W. Physiologic reactions during profound hypothermia with cardioplegia. Anesthesiology 1961; 22:87381.
Frei C, Darocha T, Debaty G, et al. Clinical characteristics and outcomes of witnessed hypothermic cardiac arrest: a systematic review on rescue collapse. Resuscitation 2019; 137:418.
Wood S. Interactions between hypoxia and hypothermia. Annu Rev Physiol 1991; 53:7185.
Podsiadlo P, Darocha T, Svendsen OS, et al. Outcomes of patients suffering unwitnessed hypothermic cardiac arrest rewarmed with extracorporeal life support: a systematic review. Artif Organs 2020.

